Hernia
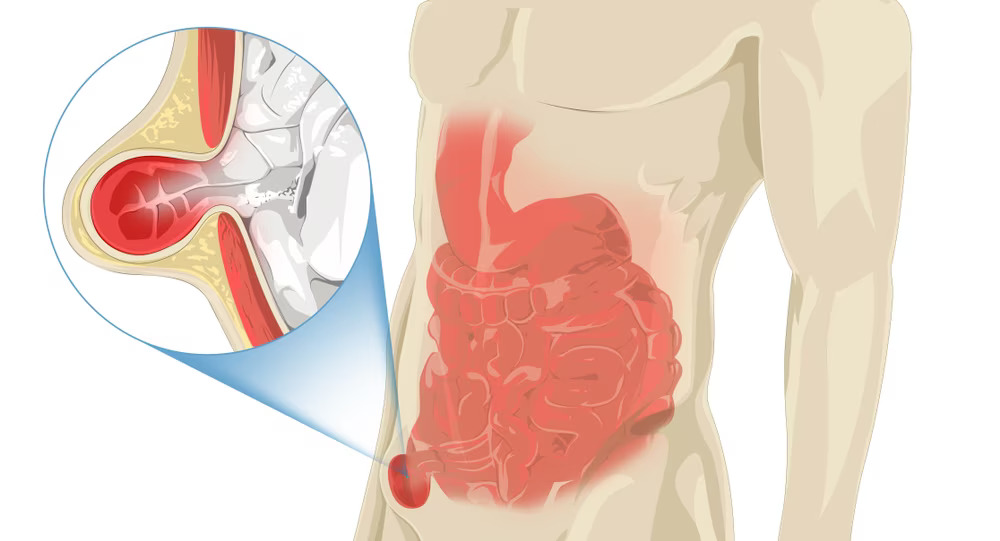
Hernia
Hernias manifest as bulges or protrusions in the abdomen or groin area, typically exacerbated by physical activity, coughing, or straining. Common symptoms include a visible lump or swelling, discomfort or pain, especially when lifting heavy objects, bending over, or coughing. Some individuals may also experience a sensation of heaviness or pressure in the affected area.
Causes:
Hernias occur when an organ or fatty tissue pushes through a weak spot or tear in the surrounding muscle or connective tissue. Various factors contribute to hernia development, including congenital weaknesses in the abdominal wall, persistent coughing or sneezing, heavy lifting, obesity, pregnancy, or chronic constipation. Additionally, previous surgical incisions or abdominal trauma can increase the risk of hernias.
Treatment
Treatment for hernias typically involves surgical intervention, although watchful waiting may be an option for asymptomatic or minimally symptomatic hernias. Surgery aims to repair the weakened area of the abdominal wall and reinforce it to prevent recurrence. Common surgical techniques include open repair and laparoscopic repair. During open repair, the surgeon makes an incision near the hernia site, pushes the protruding tissue back into place, and reinforces the weakened area with sutures or mesh. Laparoscopic repair involves making several small incisions through which a tiny camera and specialized surgical tools are inserted to perform the repair. Recovery time varies depending on the surgical approach and individual factors but generally involves a gradual return to normal activities under the guidance of a healthcare provider.
In conclusion, recognizing the symptoms of a hernia and seeking timely medical evaluation is crucial for prompt diagnosis and appropriate treatment. With advances in surgical techniques and personalized care, individuals with hernias can undergo successful repair and achieve improved quality of life.

